Sclerotherapy
About Sclerotherapy in New Jersey
In the sclerotherapy procedure a sclerosant is injected into unwanted superficial blood vessels, typically on the legs, to eliminate them. Although lasers, such as the GentleYAG and V-Beam, are also widely used for the treatment of leg vessels, sclerotherapy remains the gold standard to which other treatments are compared.
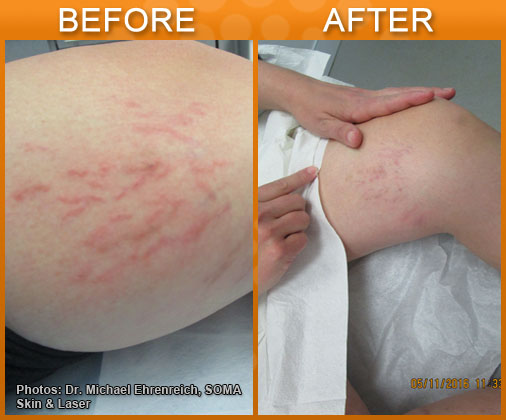
Disclaimer: Results may vary patient to patient. There is no guarantee that any specific result can be achieved. Results may not be permanent.
When considering lower extremity blood vessels, they are divided based on size and color:
- Telangiectasias are blood vessels less than 1 mm in diameter, flat and red.
- Venulectasias are blue vessels, less than 2 mm, sometimes elevated above the skin surface.
- Reticular veins are larger, 2-4 mm blood vessels, with a dusky blue/purple hue.
Sclerotherapy can improve the appearance of these blood vessels and also may reduce symptoms, such as pain or burning, if present. Generally, large varicosities are not as amenable to sclerotherapy as small ones.
Ultrasound and sclerotherapy
Most sclerotherapy is performed visually, based on the clinicians evaluation of the blood vessels, but duplex ultrasound is sometimes employed to visualize the blood vessels while injecting.
Ultrasound evaluation is sometimes necessary prior to treatment to determine the extend of underlying venous disease.
Choice of sclerosing agents
The goal of sclerotherapy is to damage the injected blood vessel and not damage the surrounding skin or tissue. Sclerosants are categorized based on their method of action.
Detergents
Detergents disrupt the cellular membranes of the cells lining the veins. These agents include: Sodium tetradecyl sulfate (Sotradecol), Polidocanol (Asclera), Sodium morrhuate (Scleromate), and Ethanolamine Oleate (Ethamolin). Detergents can be foamed by mixing with air, and this form of sclerosant is commonly used, especially for larger vessels.
Osmotic agents
Osmotic agents damage the cells by creating an electrolyte gradient, thereby dehydrating the cells. The classic hypertonic sclerosant is hypertonic saline or hypertonic saline with dextrose (Sclerodex).
Chemical agents
Chemical agents directly damage the cells in a caustic fashion. These agents include chromated glycerin (Sclermo) and polyiodinated iodine.
Of the above sclerosants, hypertonic saline, sodium tetradecyl sulfate, and polidocanol are most commonly used.
Hypertonic Saline
Hypertonic saline (23.4%) is readily available, nontoxic, and inexpensive. It is widely used off-label for sclerotherapy but has some drawbacks. If it gets outside the blood vessel it can cause pain, burning or cramping. It is also likely to cause hemosiderin deposition and hyperpigmentation. Nevertheless, it is a good option for some, especially if cost is a factor. For larger veins, 23.4% saline is usually used, while telangiectasias are usually treated at half strength (11.7%).
Sodium Tetradecyl Sulfate
Sodium Tetradecyl Sulfate is a synthetic detergent, and is FDA-approved for sclerotherapy in the U.S. as Sotradecol. The main issues with Sotradecol use are hyperpigmentation, tissue necrosis if it gets outside the blood vessel, and occasional allergic reactions, including anaphylaxis. Concentrations used range from 0.25-0.4% for reticular veins and venulectasias and 0.1-0.2% for telangiectasias.
Polidocanol (Asclera)
Polidocanol (Asclera) is FDA-approved in the United States for sclerotherapy. Notable advantages are that it does not cause tissue necrosis if extravasated, is painless upon injection,and has a low incidence of allergic reaction, though cases of anaphylaxis has been reported. As with other agents, hyperpigmentation sometimes occurs. Concentrations of 0.5-1.0% are used for for reticular veins and venulectasias and 0.25-0.75% for telangiectasias.
The sclerotherapy procedure
After a pre-operative evaluation and consent, the patient is positioned appropriately and the sclerosant injected into the blood vessel using a 30G needle, typically 0.1-0.2 ml at 2-3 cm intervals along the vessel. Larger vessels are treated first and then smaller ones. Pressure with taped cotton balls or a compression garment are applied immediately, and should be continued for several weeks.
Complications of sclerotherapy
Complications can occur with sclerotherapy. Hyperpigmentation is common and usually resolves over time. Allergic reactions can occur during treatment. Telangiectatic matting (a collection of new small vessels) sometimes occurs, and is thought to be due to injections that are too fast or too concentrated or to the presence of unrecognized feeder vessels. These sometimes resolve spontaneously, but are also amenable to treatment, often with laser. An important potential complication is tissue necrosis, usually occurring when the sclerosant escapes or is injected into surrounding tissue, or injected into an arteriole. Immediate white blanching is an indication of impending necrosis. This can be treated with massage, topical nitroglycerine paste, hyaluronidase injection, or flushing with normal saline or lidocaine. Superficial thrombophlebitis (inflammation of the veins) can occurs when larger vessels are treated. This usually responds to compression and NSAIDs. Deep venous thrombosus sometimes occurs, and must be treated with systemic anticoagulation. In addition to the above, foam sclerotherapy has unique possible adverse effects that can result from migration of foam bubbles. These include pulmonary symptoms, visual and neurological events.

