Psoriasis
Psoriasis Treatment in New Jersey
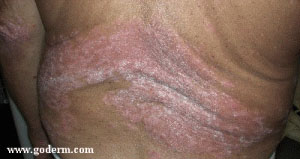
Psoriasis is an inflammatory rash of characterized by rapid epidermal proliferation with scale. The lesions are sharply demarcated, erythematous plaques or papules, with a silvery scale. Favored sites include the scalp, elbows, knees, and intergluteal cleft. Lesions in intertriginous areas (body folds) typically lack scale due to moisture in the area and the resulting maceration. Pruritus is variable, ranging from mild to severe.
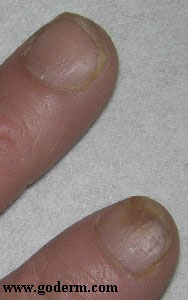
Nail involvement is present in approximately half of psoriasis patients, with changes that include “ice pick” pitting and onycholysis (separation of the nail plate from the nail bed.) Fingernails are affected more frequently than toenails. All nails or only some may be affected. Nail changes are usually asymptomatic, but can be of considerable cosmetic concern. Joint involvement and psoriatic arthritis also may coexist with the skin manifestations of psoriasis.
The onset of psoriasis is usually gradual, though variants exist with rapid onset of numerous lesions. Guttate psoriasis-the sudden appearance of multiple small psoriatic lesions-is frequently preceded by streptococcal infection of the throat. Suddenly worsening or new onset psoriasis may be associated with AIDS. A history of the Koebner Phenomenon (trauma precipitating a psoriatic lesion) may be present. Emotional stress also seems to contribute to flares. Drugs may sometimes be implicated in the disease, especially lithium, beta blockers, and NSAIDs. Pustular psoriasis is a rare form of the disease characterized by either pustules on typical plaques, pustules on the palms and soles, or a generalized pustular eruption along with fever and leukocytosis (elevated white blood cells).
With what can psoriasis be confused?
On the scalp, psoriasis is often confused with seborrheic dermatitis. Guttate psoriasis can resemble pityriasis rosea. Early lesions or those in intertriginous areas that lack scale may be less confidently diagnosed. Intertriginous lesions can resemble intertrigo or fungal infections. Nail involvement may be difficult to distinguish from fungal infection; signs of psoriasis at other commonly involved sites should be sought. Subacute cutaneous lupus erythematosus is also a consideration.
How is psoriasis diagnosed?
Diagnosis is usually self-evident based upon the typical appearance and distribution. Biopsy is usually not necessary. A family history is present in approximately one third of patients.
The typical nail appearance is pitted with brown (“oil stain”) discolorations. Other findings include oncyholysis (separation of the nail plate from the nail bed), fragility and crumbling of the distal nail, and splinter hemorrhages. To distinguish psoriatic nail disease from fungal infection, a KOH preparation or fungal culture may be necessary. Rarely, a nail biopsy will be necessary.
Patients with psoriatic skin lesions should be questions regarding a history joint pain or swelling.
How is psoriasis treated?
The mainstay of therapy are agents that decrease epidermal proliferation and dermal inflammation. Biologic medications block various immune system pathways that have been implicated in psoriasis. The following agents/modalities are used:
Topical steroids
High potency steroids are good agents for limited areas of involvement. Over-the-counter preparations are generally ineffective; prescription strength is required. A positive response is usually evident within a few weeks. Intermittent usage is recommended, since continued use of steroids can result in a loss of therapeutic effect (i.e. tachyphylaxis). Skin atrophy is a potential complication. Systemic steroids should be avoided due to long-term side effects and the propensity for disease rebound with drug discontinuation.
Topical tars/anthralin
These compounds are hydrocarbons with anti-mitotic and anti-inflammatory activities. These agents take longer to produce a response than do steroids, but the remittance is often longer lasting. Tachyphylaxis is less common with these agents than with steroids. Tar oil (e.g. Cutar) added to bath water is a convenient way to apply the drug to large surface areas. The preparations can temporarily stain skin and permanently discolor fabrics and plastic bathtubs. The addition of salicylic acid may be helpful to reduce scale. Anthralin preparations (e.g. Drithocreme and Micanol) are potentially irritating. It is started at low concentrations and advanced as tolerated.
Calcipotriene
Calcipotriene (e.g. Dovonex) is a topical vitamin D derivative with anti-mitotic activity. Vitamin D3 analogues are a mainstay of treatment for psoriasis, alone or in combination with a topical steroid. It requires several months to reach full effect. It may cause irritation. Calcipotriene can also be found in combination with a steroid in some products (e.g. Taclonex)
Tazarotene
Tazarotene (e.g. Tazorac) is a retinoid that selectively binds RAR-beta and RAR-gamma receptors. It decreases epidermal proliferation and inhibits psoriasis-associated differentiation. It is usually a second line therapy for psoriasis, either alone or in combination. It is applied at bedtime (so as to avoid sun exposure afterward) and often used with a steroid applied by day, which helps reduce the irritation that is sometimes caused by retinoids. It is pregnancy category X and contraindicated in women that may become pregnant.
Ultraviolet B light (UVB)
UVB in the 311-313 nm band in erthymogeneic doses is the most optimal irradiation therapy available today. Ultraviolet light can be provided by special light sources and lasers, in the doctor’s office or as a home unit, or from natural sunlight. It can be used in conjunction with tar/anthralin products or other topical treatments..
Psoralen and ultraviolet A (PUVA)
For widespread disease resistant to topical therapy, psoralens and UVA may be effective. Psoralens intercalate with DNA and form adducts during UVA irradiation. Long-term use increases the risk of developing skin cancer.
Methotrexate
Methotrexate is an anti-metabolite that inhibits cellular proliferation. It is usually administered weekly. It is highly effective, but has numerous side-effects, especially liver toxicity. Currently elevated liver enzymes, cirrhosis or recent hepatitis are contraindications, as is excessive alcohol intake. Liver biopsy is the gold standard for pre-methotrexate screening and screening during use, but this is less often performed today. Substantial liver damage can occur even without an elevation in liver enzymes or signs of liver failure. Folic acid supplementation can be used to reduce some side effects of methotrexate. Methotrexate is cleared renally and is contraindicated in sever renal failure. Frequent laboratory follow-up is required.
Acitretin
Acitretin is an oral retinoid that is effective for psoriasis. It has numerous side-effects. It is pregnancy category X and contraindicated in women that may become pregnant.
Cyclosporine
Cyclosporine, a T-cell suppressing drug used to prevent transplant rejection, is also effective in psoriasis. Nephrotoxicity (kidney damage) is its main side-effect. It should be used in several month courses, alternated with other therapies, to reduce the risk of renal damage.
Biologics
Severe psoriasis is often treated with immune-modulating drugs such as Enbrel, and Humira, which are TNF-blockers. This class of medications must be injected. Newer biologics include Cosentyx, Talz, Siliq, Skyrizi, Stelara, Tremfya, and Ilumya. IL-23 and IL-17 are the most recent targets of biologics.
Psoriatic arthritis is usually treated with a biologic, or with methotrexate or nonsteroidal anti-inflammatory drugs (which are also a potential cause of worsening psoriasis).
Treatment of the nail manifestations of psoriasis is usually unsuccessful without systemic treatment. Topical preparations are ineffective; steroid injections into the ail bed are painful. Systemic therapies, as described above, will often benefit the nail involvement. However, involvement limited to the nails usually would not justify the use of treatments with a high potential for toxicity. Cosmetic improvement can be achieved with manicures, nail polish and artificial nails.
What is the prognosis for psoriasis?
Psoriasis is a chronic condition with a waxing and waning course that can usually be controlled with the therapies discussed above. It can cause social isolation and psychological problems. It tends to improve in the summer, possibly due to sunlight, and worsen in winter. Secondary infection can occur. Rarely, widespread psoriasis can be a cause of erythroderma, and its life-threatening complications. Psoriatic arthritis affects approximately 5% of psoriasis patients, in various patterns: distal interphalangeal joints; asymmetric small and medium-sized joints; rheumatoid arthritis-like; ankylosing spondylitis; and arthritis mutilans. Nail involvement is often associated with arthritis of the distal interphalangeal joint. Like the underlying disease, nail involvement is a chronic condition.

