Facial Filler Injections in New Jersey For Facial Rejuvenation
Contact SOMA Skin & Laser at 973-763-SKIN (7546) for a dermal skin filler consultation
At SOMA Skin & Laser, we offer cutting-edge dermal filler treatments to help you achieve a refreshed and youthful appearance. Dermal fillers are a non-surgical solution to restore volume, smooth fine lines and wrinkles, and enhance facial contours, giving you a naturally rejuvenated look.
What Are Dermal Fillers?
Dermal fillers are injectable treatments made from hyaluronic acid and other biocompatible substances. These fillers work by replenishing lost volume in the skin, smoothing out wrinkles, and enhancing facial features. Common areas treated include:
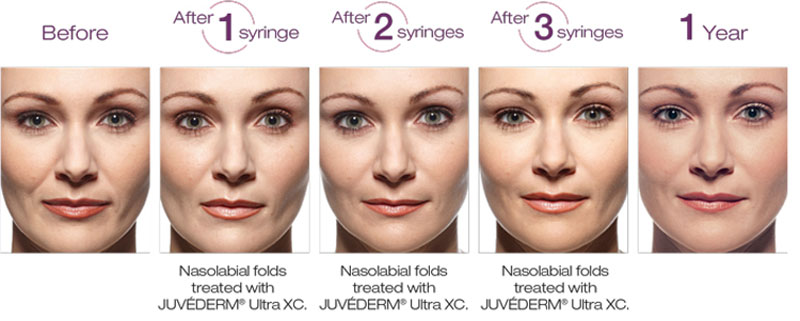
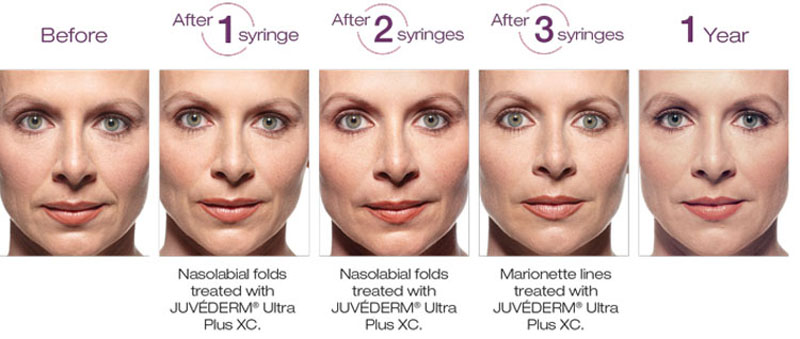
- Nasolabial folds (smile lines)
- Marionette lines
- Cheeks
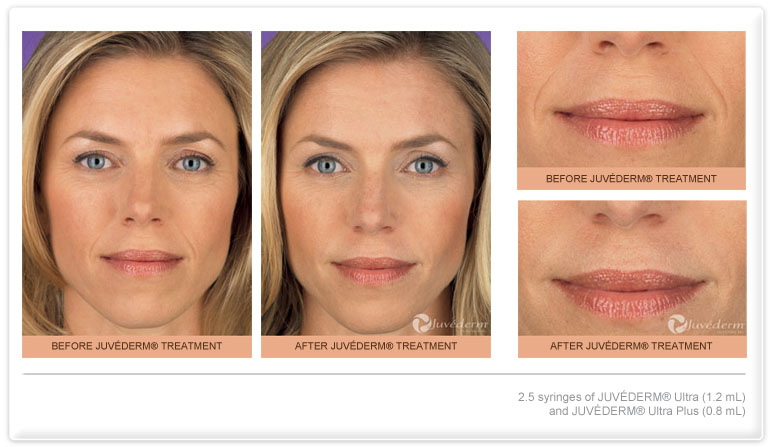
- Lips
- Chin and jawline
- Under-eye hollows (tear troughs)
- Hands
SOMA Skin & Laser offers facial filler injections, such as Juvederm Voluma, Juvederm Ultra, Juvederm Ultra Plus, Juvederm Volbella, Juvederm Vollure, Restylane, Belotero and Radiesse, for rejuvenation and the treatment of wrinkles. Many facial fillers (including Juvederm products, Restylane and Belotero) are a form of hyaluronic acid. Hyalronic acid is a naturally occurring substance in the body, which can be injected to smooth wrinkles and restore youthful volume. Injection of facial fillers, such as Juvederm, is one of the most popular non-surgical cosmetic procedures in the United States.
Benefits of Dermal Fillers
- Immediate Results: Noticeable improvements are visible right after treatment, with full results in 1-2 weeks.
- Minimal Downtime: Most patients return to daily activities right after the procedure.
- Long-lasting Effects: Depending on the filler type, results can last from 6 months to over a year.
- Natural Look: Our skilled injectors use advanced techniques to provide subtle, natural-looking results that enhance your features.
Our Filler Options
We offer a variety of dermal fillers tailored to meet your individual needs. Some of the most popular filler brands we use include:
- Juvederm: Ideal for adding volume and smoothing wrinkles around the mouth, lips, and nasolabial folds.
- Radiesse: Stimulates collagen production and is ideal for deeper lines and wrinkles.
- Sculptra: Encourages natural collagen growth, providing gradual and long-lasting results.
The Treatment Process
Our experienced dermatologists will begin with a consultation to understand your aesthetic goals. After a thorough evaluation, we will recommend the right type of filler and injection technique to achieve the best results.
In the facial filler injection procedure, the skin filler material is injected into areas that require volume enhancement. This can be a specific wrinkle or defect, or the entire mid-face to restore the rounded contours of youth. The lips are commonly treated with skin fillers to restore volume lost to aging and create a fuller lip. The most commonly treated areas are the wrinkles around the mouth and nose (nasolabial fold), the mid-face (cheeks), and lips, but other areas and defects can be treated as well. With Belotero and Juvederm Volbella finer, more superficial lines can be treated as well, such as vertical lip lines or the tear trough area. For more lift, such as the cheeks, Voluma is a good choice. Voluma is intended for deep placement to correct age-related volume loss in the midface. With optimal treatment, natural-looking results last up to 2 years. Radiesse provides more lift than most hyaluronic acid fillers, and is especially useful in the mid-face and cheeks, but unlike hyaluronic acid fillers, Radiesse cannot be dissolved.
Skin filler injections are done with a fine needle. Some skin fillers, such as Juvederm products, contain a local anesthetic, while for others a topical anesthetic agent or ice may be applied first to the skin for numbing.
Post-Treatment Care
While dermal filler treatments are minimally invasive, some mild swelling, redness, or bruising may occur, but these side effects typically resolve within a few days. We provide post-care instructions to ensure the best outcome and are available for follow-up if needed.
Dermal Fillers For Men
Men can benefit from soft tissue fillers, such as Juvederm or Belotero, to restore volume, especially in the mid-face area and at the nasolabial folds. Men can also benefit from augmentation of the jawline, creating a more masculine firmer jawline. Augmentation of the brow to create a stronger more masculine appearance is also popular.
Why Choose SOMA Skin & Laser?
- Expertise: Our board-certified dermatologists are highly experienced in facial anatomy and aesthetics, ensuring safe and precise treatments.
- Personalized Care: We take a customized approach, focusing on your unique facial structure and goals for natural results.
- State-of-the-Art Techniques: We stay updated with the latest advancements in dermal filler technology and injection techniques for optimal outcomes.
Book Your Consultation Today!
Revitalize your appearance with our dermal filler treatments at SOMA Skin & Laser. Whether you’re looking to smooth fine lines, restore volume, or enhance your features, we are here to help you achieve beautiful, youthful results.
Contact us today at 973-763-7546 to schedule your consultation and discover how dermal fillers can transform your look.