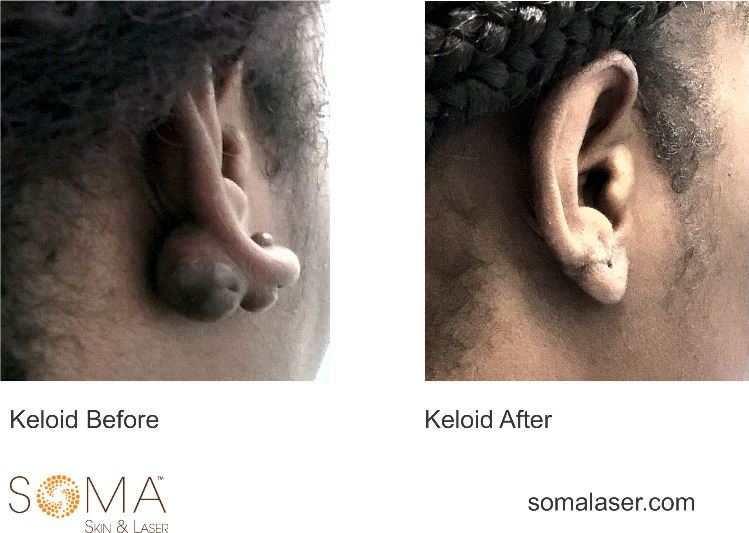
Keloid excision in New Jersey
At SOMA Skin & Laser we specialize in keloid treatment, especially of the ear. We address keloids using a combination of surgery, laser and injections, with the goal of reducing the keloid, improving appearance, and minimizing the risk of recurrence.
CALL 973-763-7546 to schedule a keloid consultation today.
About keloids
A keloid is the result of an exuberant response to skin trauma that leads to excess collagen deposition (i.e. scar tissue). It is on a continuum of normal wound healing, hypertrophic scar and keloid. It develops weeks to months after the antecedent trauma, which may be as trivial as ear piercing or an acne lesion. High-risk injuries include burns and ear piercing. Itching is common in developing keloids. Commonly affected sites are the back, upper chest, deltoid, and earlobes. They are more common in young black people. Other risk factors include: increased wound tension on a surgical wound, infection, and use of the retinoid isotretinoin. A keloid appears as excessive scar tissue that has overgrown the boundaries of the original wound. Keloids are firm and elevated with irregular borders and pink to brown in coloration.
With what can a keloid confused?
A hypertrophic scar is confined to the footprint of the original trauma, whereas a keloid, by definition, extends beyond the original confines. Dermatofibrosarcoma protuberans, a slowly enlarging fibrous tumor with low metastatic potential, can resemble a keloid. However, there is no history of antecedent trauma.
How is a keloid diagnosed?
Keloids are usually diagnosed clinically. If there is any doubt, biopsy is warranted.
How is a keloid treated?
Surgery alone is contraindicated in the treatment of keloids, as the resultant wound healing response may result in an even larger keloid. Surgery can be considered with other therapies, such as monthly intralesional steroid injections with triamcinolone, or low dose radiotherapy. These may cause flattening of the keloid. Post-surgery, pressure dressings can reduce keloid recurrence. Silicon gel dressings when worn for an extended period of time (e.g. several months) can flatten keloids and hypertrophic scars. Cryotherapy has been useful, particularly for smaller lesions. Various topical therapies, including imiquimod cream, have been used with variable success. The pulsed dye laser has been shown to be beneficial in treating keloids. Intralesional injections of various agents, such as verapamil, fluorouracil, bleomycin, and interferon alfa-2b, may also be effective. Superficial radiation therapy is used as well, but specialized equipment is required.
What is the prognosis for a keloid?
Keloids generally reach a stable size. Untreated, they are not likely to regress. With treatment a keloid may regress but will not achieve the tone or texture of normal skin.