Call 973-763-7546 For Your Vitiligo Consultation
Treating vitiligo in New Jersey
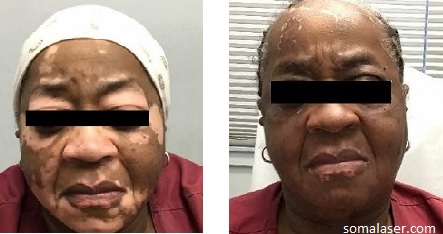
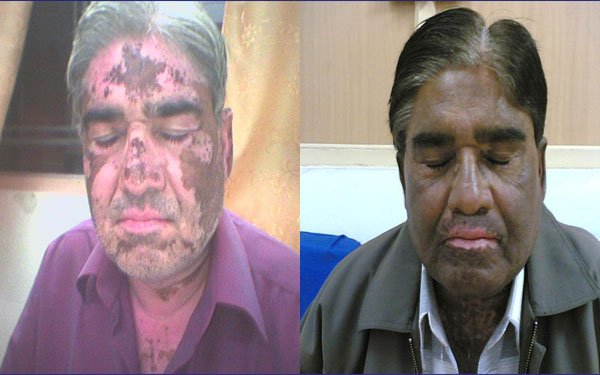
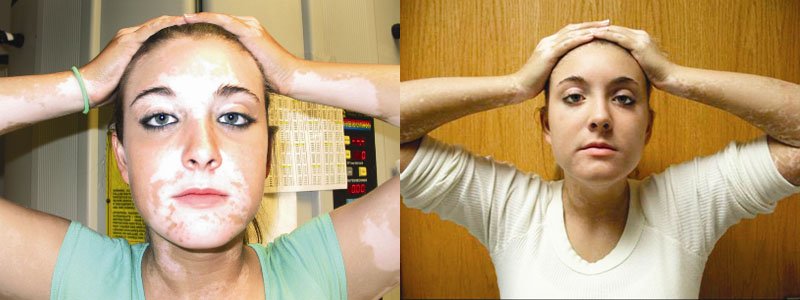
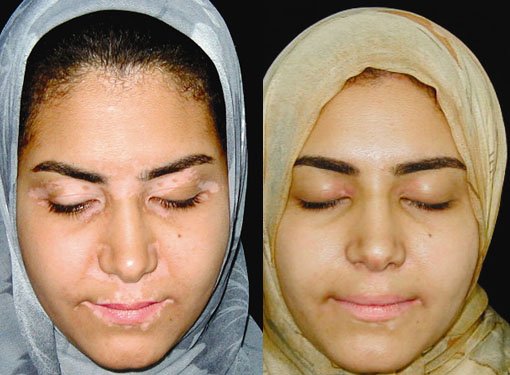
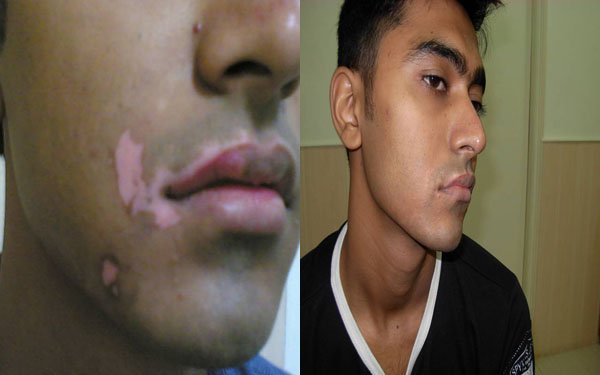
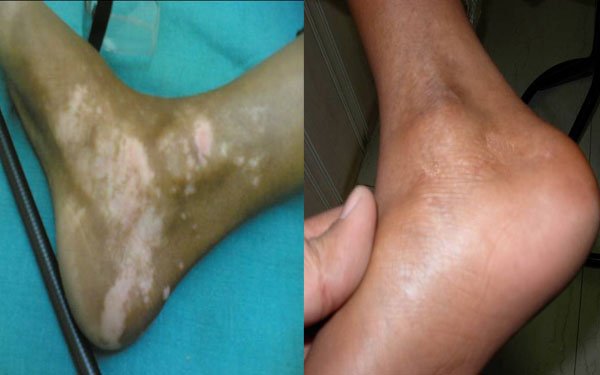
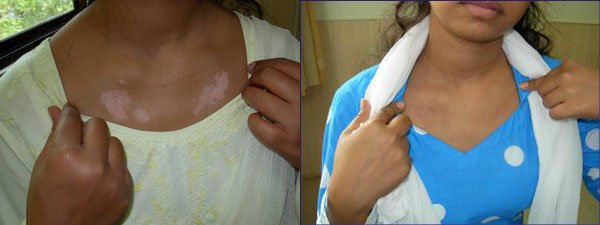
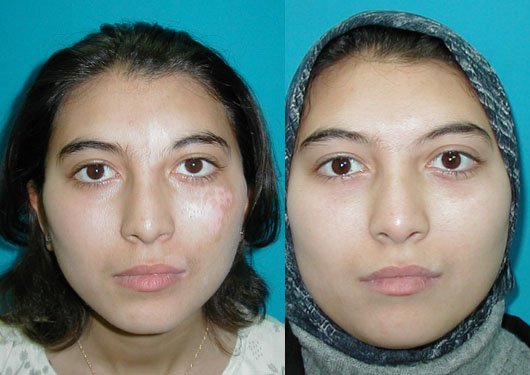
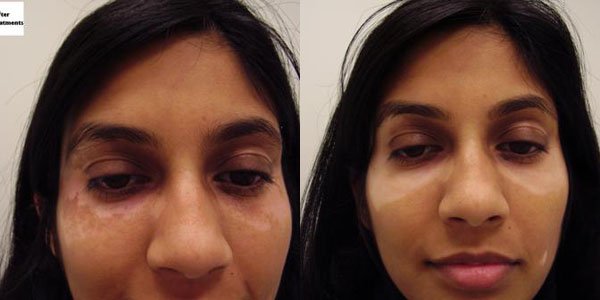
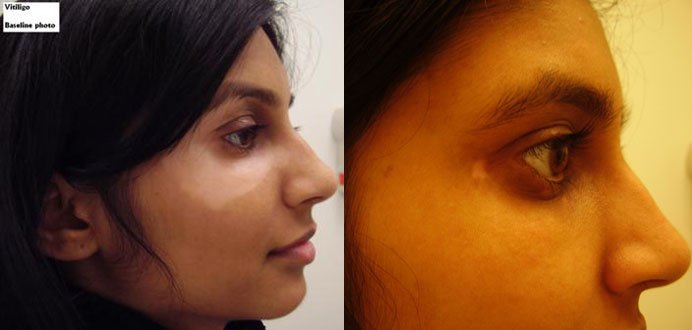
At the SOMA Skin & Laser Center for Vitiligo we treat vitiligo with a combination of medications and laser treatments.
Disclaimer: Results may vary patient to patient. There is no guarantee that any specific result can be achieved. Results may not be permanent.
About vitiligo
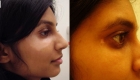
Vitiligo is a disorder that appears as sharply demarcated, round or oval, completely white macules without scale. Menaloncytes (the cells that create melanin pigment) are depleted from the affected areas. Vitiligo typically starts as one or more small white spots that enlarge over time, possibly becoming confluent. The most commonly involved areas for vitiligo are the extensor surfaces (e.g. back of hands, elbows, knees) and periorificial areas (e.g. perioral, perirectal, perioccular). The cause of the disease is unknown.
With what can vitiligo be confused?
The absence of scale distinguishes vitiligo from pityriasis alba and tinea versicolor. Vitiligo may also be confused with postinflammatory hypopigmentation. Other depigmented lesions include nevus depigmentosus and nevus anemicus.
How is vitiligo diagnosed?
Vitiligo is usually diagnosed clinically; biopsy is usually not required. On Wood’s light examination, the lesions of vitiligo will appear “chalk white”; other less obviously affected areas may be revealed as well. The conditions is generally asymptomatic. Patients seek medical care for cosmetic concerns. It may be warranted to screen for thyroid disease, pernicious anemia and Addison’s disease, which are occasionally associated with vitiligo.
How is vitiligo treated?
The goal of therapy for vitiligo is to improve cosmetic appearance. Unfortunately, treatment for depigmentation is prolonged and in most cases not fully effective. Treatment with psoralen plus ultraviolet A (PUVA) is sometimes helpful, but numerous sessions are required. Narrowband UVB phototherapy, or the 308nm excimer laser, may also be helpful, particularly in combination with calcipotriol cream. High potency steroids (e.g .clobetesol) can be helpful for limited disease. Calcineurin inhibitors (e.g. topical pimecrolimus and tacrolimus) have been shown to be safe and effective; these agents are especially useful on the face where high potency topical steroids may cause skin atrophy. Cosmetic management with camouflage makeup (e.g. CoverMark, Dermablend) is useful either alone or as an adjunct to other treatments. Sunscreen over the depigmented area is important to prevent sunburn. Needling has also been shown to be helpful in stable refractory vitiligo. Operative treatment in the form of skin grafts and punch grafts are sometimes used.
A new class of medications, the JAK inhibitors, is now approved for treating vitiligo. Xeljanz is an oral JAK inhibitor, while Opzelura is topical. Other JAK-kinase inhibitors are in the pipeline, both oral and topical.
For active disease which is progressing rapidly, stabilization with systemic steroids can be considered. Intramuscular kenalog injections is one approach. Oral min-pulse therapy with Dexamethasone is also commonly utilized. In this technique low-dose Dexamethasone (e.g. 2 to 4 mg) is given on two consecutive days each week for up to three months.
Antioxidants are sometimes used to treat vitiligo, though data are sparse. Vitamin D, alpha lipoic acid, and Vitamin C are often utilized.
What is the prognosis for vitiligo?
Vitiligo is most often a chronic progressive disease. It may sometimes progress to complete body depigmentation. In some patients, repigmentation spontaneously occurs, but it is usually incomplete. Depigmentation of the retina occurs in up to 30% of patients. Uveitis occasionally occurs as well. Autoimmune thyroid disease, especially Graves disease and thyroiditis, are sometimes associated with vitiligo, as are pernicious anemia, Addison’s disease, and alopecia areata.
Contact SOMA Skin & Laser for a vitiligo consultation in New Jersey today. 973-763-7546
More on vitiligo
| Image links | Other useful links |
| DermetnNZ: Multiple vitiligo images | National Vitiligo Foundation Seung-Kyung, H. Vitiligo. e-medicine. April 14, 2005 |